Boy, oh boy, do I have a lot of interesting data to share these days. Although COVID has driven a lot of it, I've finally been able to dig into some things that have been bugging me forever with the help of my team. Finally, I think we'll have both -25 modifier and after-hours codes benchmarks!
Until then, let's look at this interesting tidbit. Here, we have the volume of "telemedicine" based visits (whether done via video, phone, or portal) relative to the overall volume of sick visits. There's a lot to talk about here. Click on the graph to pull up a larger version.
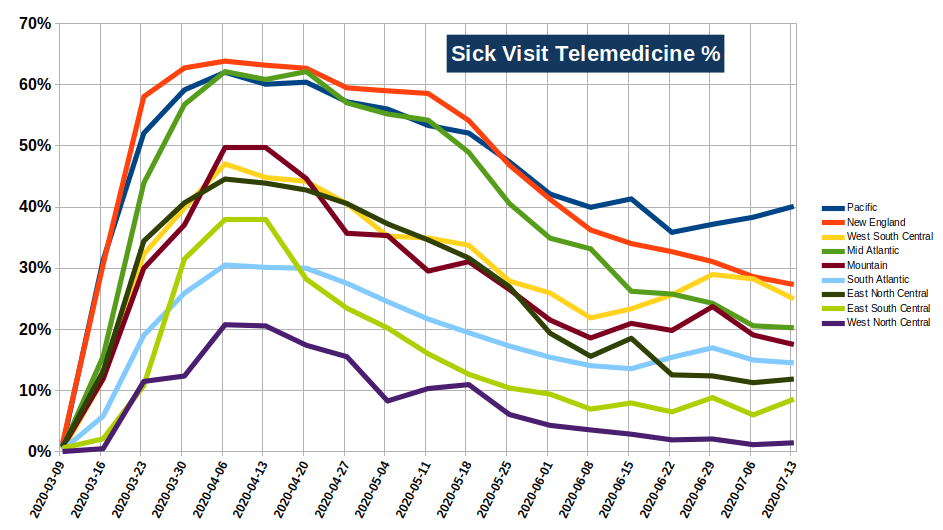
Before I begin, let me review what how the Feds sort these regions:
| East North Central |
IL |
| |
IN |
| |
MI |
| |
OH |
| East South Central |
AL |
| |
KY |
| |
MS |
| |
TN |
| Mid Atlantic |
NJ |
| |
NY |
| |
PA |
| Mountain |
AZ |
| |
CO |
| |
NM |
| |
NV |
| |
UT |
| |
WY |
| New England |
CT |
| |
MA |
| |
NH |
| |
VT |
| Pacific |
CA |
| |
OR |
| |
WA |
| South Atlantic |
DC |
| |
DE |
| |
FL |
| |
GA |
| |
MD |
| |
NC |
| |
SC |
| |
VA |
| West North Central |
KS |
| |
MO |
| |
NE |
| West South Central |
LA |
| |
OK |
| |
TX |
Things we notice:
- The hardest hit parts of the country (or those places where shutdowns were most effectively enforced) generally had the highest rates of telemedicine visits. California/Washington, New England, and the NY-NJ-PA route. The least hit part of the country (West North Central) has the least telemedicine use. However, that changes as the Mid Atlantic states see their COVID efforts drop and the West South Central, driven primarily by Texas, sees more COVID and, therefore, more telemedicine.
- When I looked at this last in June, it appeared that telemedicine had fallen off universally as states and businesses began to open back up. A lot of our practices were clearly doing their best to go "back to normal." Well, after that first week in June, a number of regions saw their telemedicine rates rise. 6 of the 8 regions saw increases in that last week of June.
- Many of the major payors have announced that telemedicine payments will end in July, others shortly thereafter. If you're not screaming about telemedicine coverage, time for your voice to join the chorus.
We don't know what the new normal is yet and the longer that this volume of telemedicine sticks around, the more normal it will become. Study after study shows that parents prefer telemedicine visits in many circumstances. Time for us to figure this out.
Comments
4 Comments